1 – Establish Trust
Youth must feel safe to engage in conversations around substance use prevention. You can create a welcoming and safe environment by building trust and rapport, engaging parents/guardians when appropriate, keeping confidentiality at the forefront and staying up-to-date on best practices.
Building Trust and Rapport with Youth
Having conversations with youth about substance use can be difficult. It’s important to first establish a trusting relationship that fosters open communication and encourages active engagement and receptiveness to sensitive topics related to substance use.
The best way to acknowledge varying backgrounds and identities is to have a respectful and open conversation. This will help to establish boundaries and provide a general sense of the youth’s perspective.
Check out this quick video to learn more about building trust and rapport with the youth you serve.
This Building Trust and Rapport with Youth Guide includes additional steps that youth-serving providers can take to build trusting and meaningful relationships with the youth they serve. Building and maintaining relationships with youth is essential to gaining their trust. It is important to note that this guidance should be adapted to fit each relationship accordingly, as one size does not fit all.
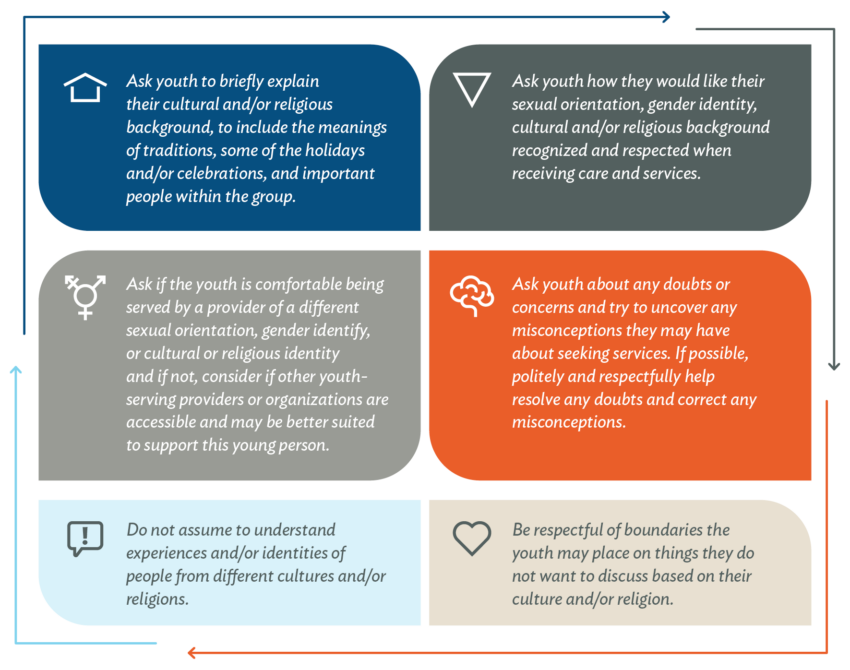
Written by one of our Youth Ambassadors, the following tips can help youth-serving providers approach such a conversation.
Confidentiality and Parental Involvement
Guidance and resources for understanding confidentiality when navigating discussions with youth and their parents/caregivers.
Communication Pathway
The purpose of this worksheet is to guide you through a few simple communication steps that can be tailored to any circumstance.
Prevention Language Guide
Language is powerful. Words impact the way individuals interpret ideas, perceive intentions and view the world around them. The words we choose to use matter. This is especially true when talking about substance use. That’s why it’s important to use non-stigmatizing, person-first language to reduce stigma and negative bias. This guide, Language Matters When Discussing Substance Use, outlines how to incorporate non-stigmatizing language into your conversations with young people.
LGBTQ+ Affirming Care
Finding the right provider is important for one’s physical and mental health but the process can be difficult. LGBTQ+ people have an added challenge finding a provider who supports their identity. We have provided information below and a guide to help support providers, families, and youth.
For a quick reference, view our Questions for LGBTQ+ Youth and Their Parents/Caregivers to Ask Care Providers Guide. For definitions of terms used below, or of other LGBTQ+ terms and acronyms, we recommend referring to this glossary by Michigan State University.
What Is LGBTQ+ Affirming Care?
Affirming care means a health care provider affirms (supports or encourages) their patient’s identity and recognizes how it impacts life and health. An affirming provider takes an active role in working to bridge cultural differences (American Association of Marriage and Family Therapists, n.d.). LGBTQ+ affirming providers “embrace a positive view of lesbian, gay, bisexual, transgender and queer identities and relationships and address the negative influences [of] homophobia, transphobia and heterosexism” on health and wellbeing (American Association of Marriage and Family Therapists, n.d.). LGBTQ+ affirming care is medical care that uses this approach to be respectful and empowering to LGBTQ+ clients. This type of care moves beyond neutrality and instead recognizes and affirms how LGBTQ+ identity can be connected to unique strengths, needs and concerns.
Why is LGBTQ+ Affirming Care Important?
Unique Health Needs
LGBTQ+ people often experience stigma and discrimination based on their sexual orientation, gender identity and gender presentation. The stress of this discrimination puts LGBTQ+ people at a higher risk for mental health challenges like anxiety and depression and using substances like drugs and alcohol. This high risk of health conditions means it is especially important for LGBTQ+ people to have access to health care that they feel comfortable using.
A 2023 Trevor Project survey of LGBTQ+ youth found that 67% reported experiencing symptoms of anxiety, 54% reported experiencing symptoms of depression and 41% seriously considered suicide in the past year (The Trevor Project, 2023). A separate 2015 report found that LGBTQ+ youth were 30% more likely to heavily use alcohol, 60% more likely to use cannabis, 190% more likely to inject substances and 230% more likely to use cocaine than their straight, cisgender peers (Human Rights Campaign Foundation, Partnership for Drug-Free Kids, 2015).
Mental health and substance use challenges among LGBTQ+ youth may be further exacerbated by the unique obstacles and treatment they face, including conversion therapy. Conversion therapy, also known as sexual orientation gender identity change efforts or sexual orientation change efforts, comprises methods that “aim to change a person’s same-sex sexual orientation to other-sex, regardless of whether mental health professionals [or lay individuals] are involved.” (Glassgold et al., 2009). Peer-reviewed studies of conversion therapy indicate that there is little evidence supporting its effectiveness and that many individuals experience harm from these practices. Both the American Psychological Association and American Psychiatric Association have made statements opposing conversion therapy practices since 2022 and 1997, respectively. Despite this, approximately 57,000 youth ages 13-17 in the United States will be subjected to conversion therapy before turning 18 (Mallory et al., 2019). LGBTQ+ youth who experience conversion therapy are 25% more likely to use alcohol or marijuana than LGBTQ+ youth who do not (The Trevor Project, 2022).
LGBTQ+ people may also face identity-specific health needs across their life course, such as grappling with sexual and gender identity, considering medical gender transition and exploring options for having children (Ard, K., 2016).
Barriers to Care
LGBTQ+ people sometimes experience discrimination in health care settings, either from individual providers or by systems not designed with the needs of LGBTQ+ people in mind. This can range from clients being referred to by the wrong name or gender pronouns, to the use of slurs, denial of care or even violence from providers. When an LGBTQ+ person experiences discrimination from their health care provider, they may feel unsafe, stop trusting their provider and even stop seeking out care.
According to the 2023 Trevor Project survey, of the 81% of LGBTQ+ youth who indicated they wanted mental health care, 56% were not able to receive it. Many of the respondents described fear of discrimination in health care settings as a key reason for not receiving mental health care: around a quarter cited specific factors like “fear of being outed” (27%) and “fear of my identity being misunderstood” (23%) (The Trevor Project, 2023).
Affirming care can support LGBTQ+ clients in navigating their unique needs and barriers in an empowering way.
Opportunities for Support
Role of Health Care Providers
In assessments conducted by the National Council for Mental Wellbeing in 2021 and 2022, 52% of youth identified health care providers as a trusted source of information on substance use, a finding that positions providers to have a significant impact on youth attitudes and beliefs about substance use. (Sloyer et al., 2023).However, the same respondents indicated often feeling uncomfortable speaking to providers; only 7% ranked health care providers as the adults they felt most comfortable speaking with about substance use and mental health (Sloyer et al., 2023).
Health care providers are in a valuable position to convey key information to youth and help increase trust in the medical system. Health care providers can use the guide to connect with LGBTQ+ patients’ needs and to share to the importance of LGBTQ+ affirming care. Providers can also encourage parents and caregivers to use the guide to support their LGBTQ+ youth in connecting with an affirming health care provider.
Role of Family
Though young people state that family is important to them (Sloyer et al., 2023) and can be a source of joy and support (The Trevor Project, 2022), almost half of youth surveyed say that fear of getting parent or caregiver permission is the reason they do not have access to mental health care (The Trevor Project, 2023). On the flip side, youth cited being more comfortable having difficult conversations with parents and caregivers than health care providers (Sloyer et al., 2023). This presents parents and guardians the opportunity to bridge the gap between youth and providers by helping youth access information about mental health and substance use from trusted and affirming sources. Parents and caregivers can help ease fears about receiving care by proactively supporting youth – not just when they are accessing mental health care, but also when they seek affirming care. Parents and caregivers can use this resource to support their LGBTQ+ youth in connecting with an affirming health care provider.
View our Questions for LGBTQ+ Youth and Their Parents/Caregivers to Ask Health Care Providers Guide before visiting with a health care provider.
Role of Youth
Parents and caregivers of LGBTQ+ youth may not be aware when discrimination or identity-insensitive care happens, or they may not understand the scope or negative impact of that care. They may also be unfamiliar with how to talk to providers about gender and sexuality or how to effectively question potential providers about beliefs and areas of expertise. Providers can encourage youth to use How To Find Affirming Care to work with their parent(s) to find a provider that is LGBTQ+ affirming or to reach out to providers directly if the parent or caregiver is not supportive of the youth’s LGBTQ+ identity.
This project is supported by the Centers for Disease Control and Prevention (CDC) of the U.S. Department of Health and Human Services (HHS) as part of a financial assistance award totaling $1,500,000 with 100% funded by CDC/HHS. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement by, CDC/HHS or the U.S. Government.
